- Men
- Bilateral Scrotal Orchidectomy
- Bladder Neck Incision (B.N.I.) and Urethrotomy
- Brachytherapy
- Circumcision
- Cystoscopy
- Flexible Cystoscopy
- Hydrocelectomy Spermatocelectomy & Epididymal Cystectomy
- Inguinal Orchidectomy
- Kidney Cryotherapy
- Laparoscopic Nephrectomy
- Laproscopic Pyeloplasty
- Laser Prostatectomy
- Magnetic Resonance Imaging (MRI) Scan
- Nephrectomy
- Orchidopexy
- Other Services (Men & Women)
- Other Treatments (Men Only)
- Robotic Assisted Laparoscopic Prostatectomy
- Sexual Dysfunction
- Transperineal Ultrasound Guided Prostate Biopsy (TPPB)
- Transrectal Ultrasound & Biopsies of the Prostate
- Transurethral Resection of Bladder Tumour
- Ureteroscopy
- Vasectomy
- Women
- Children
- Clinical Trials
Treatment Process:
Laser Prostatectomy
This information is designed to help you, your family and friends prepare for your surgery. It will also help you plan how to take care of yourself in the weeks following discharge from hospital.
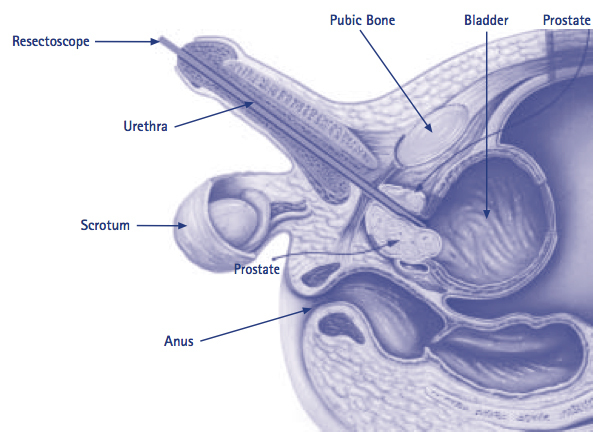
A laser prostatectomy is an operation for men who have problems passing urine because of an enlargement of the prostate gland. The prostate is a small but important gland in the male reproductive system. Its main job is to produce seminal fluid which protects and enriches the sperm. The prostate gland sits just below the bladder and surrounds the neck of the bladder and the beginning of the urethra (the canal from which you pass your urine).
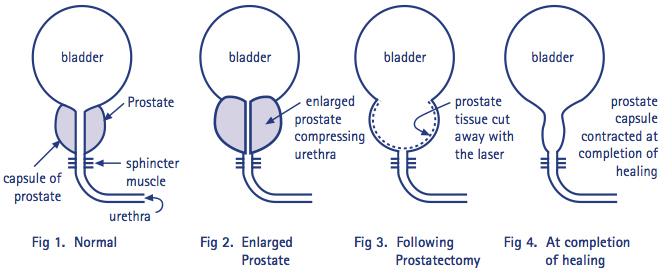
The cause of prostate enlargement is unknown but it appears to be due to changes in the levels of hormones in the blood in the aging male. When the prostate tissue enlarges inward it squeezes on the urethra causing some or all of the following symptoms:
- Frequency, (the need to void often)
- Urgency, (the need to void in a hurry)
- Nocturia (the need to get up at night to void
- Weak stream
- Incomplete emptying of the bladder.
The aim of the laser prostatectomy is to remove the prostate tissue which is causing the blockage, so you get relief of your symptoms.
If your prostate gland is squeezing on the urethra and causing obstruction, your bladder may be unable to empty itself completely. Over a prolonged period, the urine build-up can over-stretch the bladder and occasionally the urine can prevent the kidneys from draining properly.
This can lead to kidney damage and can have a large impact on your general health. Usually however, the operation is needed because of the unpleasant symptoms mentioned above.
Treatment
Using anaesthetic gel for lubrication a telescopic instrument called a resectoscope is passed up the urethra. The resectoscope has irrigation fluid flowing through it which keeps the camera view clear and flushes away blood and debris. The thin laser fiber sits within the resectoscope and the laser beam coming from the end of the fiber is used like a knife to cut away the prostate tissue back to the level of the prostate capsule. This removes any tissue causing obstruction of your urine flow.
The pieces of prostate tissue that are cut away are pushed into the bladder. They are then either flushed out through the resectoscope if they are small enough or they are removed by the ‘morcellator’. The morcellator is a mechanical device which passes through the resectoscope and while sucking the pieces of prostate tissue floating within the bladder to its tip, its blades cut the prostate tissue into tiny pieces so that they can be sucked out. Any tissue removed during surgery is collected and routinely sent to the laboratory where it is looked at under the microscope.
Once all the tissue fragments have been removed, a catheter (drainage tube that passes through the urethra into the bladder) is placed to drain your urine.
What is the effect of removal of the prostate tissue?
Since the obstructing tissue has been removed, there will be an immediate improvement in your urine flow. As the prostate cavity heals, urinary symptoms improve. In most men, the symptoms improve rapidly, but in others, the improvement in urgency, frequency and nocturia takes 2 or 3 months.
Are there any untoward effects after surgery, especially on my sex life?
This is the main fear that most men have with this operation. Approximately 10% of men may have a change in their potency (ability to have sexual intercourse). However, in the vast majority of cases the ability to have an erection and reach climax is not affected. One effect that must be accepted with this surgery is that you may have dry ejaculations. This is because one of the jobs of the prostate is to prevent the semen entering the bladder during ejaculation. After prostate tissue removal, the semen can pass freely back into the bladder, this is called retrograde ejaculation. This is completely harmless and does not affect your health in any way, it would only be a concern to men wanting to father children in the future. Up to 90% of patients may experience retrograde ejaculations, however the operation should never be regarded as a sterilisation procedure. If you are aware of these possibilities, your enjoyment of sex should not diminish and may well improve after surgery due to your other bothersome symptoms being resolved.
In a very small number of patients, approximately 2-3%, scarring can occur after surgery at the operation site as the tissues heal. Despite adequate removal of the prostate tissue, a ring of scar tissue can develop during healing at the neck of the bladder (‘bladder neck stenosis’) or within the urethra (‘stricture’), which may cause some renewed obstruction. In this unlikely event further day stay surgery would be required to cut through the ring of scar tissue using a resectoscope and the laser to open up the obstructing area. This short, simple procedure has a short recovery time.
Is there a risk that I might end up incontinent?
Incontinence, or leakage of urine without control, occasionally occurs temporarily and may last for a few weeks. Only very few patients have incontinence which lasts beyond the first few months.
If you were to have any incontinence after your operation, you would be given information and instructions about exercises that you can do to strengthen the pelvic floor muscles. These muscles help with control of your urine flow and toning these muscles helps to maintain your continence.
Your Consent
We need your permission for your operation to go ahead.
Before you sign the consent form, it is important that you understand the risks and effects of the operation and anaesthetic. Your doctor and the nurse will discuss these with you, should you have any questions, your nurse or doctor would be happy to answer these.
It would be a very rare occurrence to require a blood transfusion with this surgery. However, in the unusual event that you did need a blood transfusion and you want to refuse one, it is vital that you tell your surgeon and nurse prior to your operation.
About Your Anaesthetic
You will not be allowed to eat or drink anything for at least 6 hours before your surgery. This includes chewing gum and sweets.
There are two main types of anaesthetic used for this surgery;
- General Anaesthetic: You will be asleep throughout the operation and remember nothing of it.
- Regional Anaesthetic e.g. Spinal, Epidural or Caudal: A needle is placed into your back and a solution is injected that will numb your body from the waist down. You will be awake but may be sleepy and you will not feel the operation.
Feel free to discuss these options, and your questions with the anaesthetist.
You must not drive any vehicle or operate any machinery for 24 hours after having an anaesthetic. You will have to arrange for someone to drive you home if you go home within 24 hours of your surgery.
Your Operation
On admission, you will be informed of your approximate time of surgery and prepared for theatre by your nurse.
You may be given some tablets before theatre. These are charted by your anaesthetist and may include tablets for tension, nausea and pain prevention.
You will be escorted to theatre where you will be transferred to the theatre table. Anaesthetic staff will then insert a drip in your arm and attach various monitoring devices. Once you have been completely prepared and given your anaesthetic, surgery will begin. The operation can take anywhere from 30 minutes to more than two hours depending on the size of your prostate gland.
When the operation is completed, you will go to the recovery room for a short while where you will be cared for until you are ready to be transferred to the ward.
After Surgery
Your nurse will check your blood pressure, pulse and temperature routinely.
You may still have the drip in your arm so you get enough fluid until you are drinking normally. You can usually drink when you return to the ward and you may eat once you are tolerating fluids. Your urine will drain from the bladder, through your catheter into a bag. The urine is likely to be blood stained; this usually clears within the first 24 to 48 hours. The catheter is held in place inside the bladder by a small balloon so that it cannot slip out. Your nurse will monitor your catheter tube and the drainage from it.
Once you have recovered from your anaesthetic your nurse will help you, to get out of bed for the first time. If you have had a spinal anaesthetic, you may be asked to lie flat for several hours after returning to the ward to allow for the anaesthetic to wear off.
After surgery you may or may not experience some of the following symptoms:
- A burning sensation and the desire to go to the toilet. These symptoms are not usually caused by a full bladder but by the irritation caused by the removal of the prostate tissue with the laser. These symptoms are easily treated with mild pain relievers and medications, which change the acidity of the urine.
- A stinging or burning sensation at the tip of the penis where the catheter enters. This can be due to the instruments used during the operation and is easily relieved by applying an anaesthetic gel.
- A feeling of having a full bladder, this can be caused by blockage of the catheter tube either by a blood clot or by accidental kinking of the tube. These blockages are usually easily cleared by the nurse.
- Bladder spasms (short, sharp, grabbing pains). This is due to the bladder trying to expel the catheter because of irritation. Once again these are easily treated with medication.
Our aim is to keep you as comfortable as possible, it is important that the nurse know when the pain or discomfort starts so your symptoms can be treated and relieved as quickly and easily as possible. At all times, your nurse is there to help you, please ring your bell if you need assistance and your nurse is not nearby.
You will be asked to drink extra fluids after your surgery and for the next few days after your discharge. This helps dilute the blood in the urine, washes away debris and helps prevent infection. You should drink approximately 1500mls, which is about eight glasses of fluid per day. Water is best, but any fluid will be O.K. There is no need to drink excessive amounts of fluid; once the urine is free of blood you should drink just enough to keep your urine a pale yellow to clear colour.
If your surgery is done in the morning, you may well be able to go home on the same day. Arrangements would be made for your catheter to be taken out at home by the district nurse the following morning. You would be shown how to empty the catheter bag and care for it before going home. If you do not go home the day of your operation your catheter would be removed on the ward the morning after surgery. The catheter is removed by deflating the balloon using a special device located at the end of the catheter where it connects to the drainage bag. The catheter slides out easily once the balloon is deflated, causing little discomfort.
Once the catheter comes out you may at first have a burning sensation when passing urine. This is because urine is naturally acidic. Your nurse will instruct you about taking ural or citravascent to neutralise the urine to relieve these symptoms. If these symptoms continue for longer than a few days and are at all associated with frequency going to the toilet and cloudy, offensive smelling urine you should contact your own doctor as soon as possible as these are signs of a urine infection.
Going Home
Before leaving the ward, you will be given a discharge information letter, which contains helpful information for when you get home.
You will be given or sent an outpatient appointment usually for 4-6 weeks after your operation.
You may be given a prescription for medication to take only if specifically requested by the doctor. If you are prescribed antibiotics to take, it is very important that you complete the whole course of tablets, even if you feel better and do not think they need to be finished.
We will send a letter to your own doctor about your operation and the details of your treatment while you were in hospital.
Once Home
It takes time for the raw surface inside the prostate cavity to heal. Until it does you may have some discomfort passing urine, and experience some urgency, frequency, and nocturia. These symptoms subside as healing progresses and can be relieved with the help of mild pain relievers and other medications, which you will be informed about.
You may notice that you pass a little blood when going to the toilet; this is usually at the beginning of the urine stream. This is normal after this surgery and the bleeding may be intermittent. This is the normal process of healing and you need only be concerned if you have fresh heavy bleeding that does not stop or if your are unable to pass your urine at all which may be due to a blood clot blocking the urethra. If either of these unlikely events should occur you should contact your own doctor immediately or go to your nearest emergency department.
Continue to drink plenty of fluid if bleeding persists otherwise drink enough to keep your urine a pale yellow to clear colour.
You would be encouraged to do pelvic floor exercises if you have any problems with incontinence once your catheter is removed. Your nurse will provide further instructions about these exercises.
You can do most things after your operation except for any heavy lifting, straining or strenuous activity which should be avoided for 4 weeks after surgery. Apart from avoiding strenuous activities, you will be able to continue with your normal daily routines, as you feel able.
This is routinely a straightforward operation, after which most patients have a speedy recovery and experience little pain.
While you are in hospital, we will do everything we can to make your stay as comfortable as possible. The nursing and medical staff are always available to help with whatever needs you have. If you are worried about anything before or after your surgery, or if you have any further questions or would like more information, please do not hesitate to ask your nurse who will be more than happy to help.