- Men
- Bilateral Scrotal Orchidectomy
- Bladder Neck Incision (B.N.I.) and Urethrotomy
- Brachytherapy
- Circumcision
- Cystoscopy
- Flexible Cystoscopy
- Hydrocelectomy Spermatocelectomy & Epididymal Cystectomy
- Inguinal Orchidectomy
- Kidney Cryotherapy
- Laparoscopic Nephrectomy
- Laproscopic Pyeloplasty
- Laser Prostatectomy
- Magnetic Resonance Imaging (MRI) Scan
- Nephrectomy
- Orchidopexy
- Other Services (Men & Women)
- Other Treatments (Men Only)
- Robotic Assisted Laparoscopic Prostatectomy
- Sexual Dysfunction
- Transperineal Ultrasound Guided Prostate Biopsy (TPPB)
- Transrectal Ultrasound & Biopsies of the Prostate
- Transurethral Resection of Bladder Tumour
- Ureteroscopy
- Vasectomy
- Women
- Children
- Clinical Trials
Treatment Process:
Laproscopic Pyeloplasty
This information is designed to help you, your family and friends prepare for your surgery. It will also help you plan how to take care of yourself in the weeks following discharge from hospital.
A pyeloplasty is the removal of a stricture (narrowing) from within the upper ureter where it connects to the kidney. Pyeloplasty is usually reserved for strictures that are causing blockage and ongoing symptoms such as pain and recurrent infection or kidney damage.
Other treatments for ureteric strictures can be used with mild strictures and would have a slightly less chance of curing the problem, such as:
- Percutaneous endopyelotomy uses a telescopic instrument through the flank, into the kidney and repairing the stricture from within.
- Trans-ureteric surgery involves passing a thin telescopic instrument up the urethra, through the bladder and into the effected ureter without using any external incisions.
Treatment
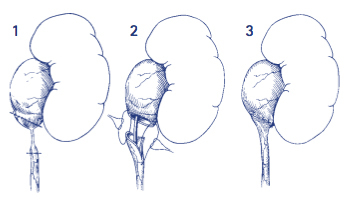
A laparoscopic pyeloplasty removes the stricture by using laparoscopic equipment. Long thin instruments are passed through five small incisions made in the flank, each about 1cm in length. The abdomen is first filled with carbon dioxide, which separates the tissues to allow for vision during the surgery. A camera is then passed, giving the urologist a detailed picture inside the abdomen. The other openings are used to pass cutting and suturing instruments so the stricture can be isolated, removed and the two remaining ends stitched together widely to prevent the stricture reoccurring.
In both cases, a wound drain is then placed to drain any ooze from the area and a nephrostomy tube may also be put in. A nephrostomy tube is a drain that is placed into the kidney through the same incision used to remove the stricture. It is stitched into place and is connected to a drainage bag that drains any urine or blood from the kidney. A ureteric stent is also placed. This thin, soft tube sits within the ureter. Both ends of the stent are curled with one loop sitting within the kidney and the other within the bladder. The stent allows healing to take place and drains the urine from the kidney. A catheter (a flexible drainage tube) is also placed through your urethra to drain your urine from the bladder into a bag and remains in place until you are up and about.
Depending on the location and length of the stricture, surgery can take anywhere from 2 to 4 hours to complete and usually involves a 2 – 4 night hospital stay for the open procedure and a 1 – 2 night stay for the laparoscopic procedure.
What are the risks involved with surgery?
With all surgery, there is a risk of infection and blood loss. The kidneys have a large blood supply and there is always some bleeding involved with surgery. In a small number of cases, a blood transfusion may be needed to compensate for blood loss during surgery.
In a small number of cases when the new join heals, scarring can occur, which can again narrow the channel within the ureter. This narrowing, known as a ureteric stricture, is usually easily treated with minor trans-ureteral surgery that opens the narrowing.
In any laparoscopic surgery, there is also the risk that the surgeon may need to proceed to open surgery, requiring a larger, single incision in the flank. This happens rarely and can be due to equipment failure, excessive bleeding or other difficulties encountered during the surgery.
Your Consent
We need your permission for your operation to go ahead. Before you sign the consent form it is important that you understand the risks and effects of the operation and anaesthetic. Your doctor and the nurse will discuss these with you, should you have any questions, your nurse or doctor would be happy to answer these.
With this surgery, there is a small chance that you may require a blood transfusion. In the unusual event that you did need a blood transfusion and you want to refuse one, it is vital that you tell your surgeon and nurse prior to your operation.
About Your Anaesthetic
You will NOT be allowed to eat or drink anything for at least six hours before your surgery. This includes chewing gum and sweets.
There are two main types of anaesthetic used for this surgery:
- General Anaesthetic: You will be asleep throughout the operation and remember nothing of it.
- Regional Anaesthetic e.g. Spinal, Epidural or Caudal: A needle is placed into your back and a solution is injected that will numb your body from the waist down. This is sometimes used in addition to the general anaesthetic to provide pain relief following the operation.
For the open pyeloplasty, if you do not have an epidural anaesthetic after your surgery you may have a P.C.A pump attached to the drip in your arm. P.C.A stands for Patient Controlled Analgesia. It is a computer-controlled machine that delivers pain relief through your drip. You will be able to control the amount of pain relief given but the anaesthetist prescribes the maximum dose. You will receive more information about the P.C.A. pump and your anaesthetic at the pre-assessment clinic.
Feel free to discuss these options and any questions with the anaesthetist.
Your Operation
On admission, you will be informed of an approximate operation time and prepared for theatre by your nurse. You maybe fitted with T.E.D. stockings that help aid circulation and prevent blood clots, which there is always a slight risk of with surgery. You may also be instructed about special deep breathing and leg exercises that you should do after surgery.
You may be given some tablets before theatre. These are charted by your anaesthetist and may include tablets for tension, nausea and pain prevention.
You will be escorted to the theatre, where you will be transferred to the theatre table. Anaesthetic staff will then insert a drip in your arm and will attach various monitoring devices. Once you have been completely prepared and given your anaesthetic, the surgical site may be shaved and surgery will begin.
When the operation is completed, you will go to the recovery room for a short while where you will be cared for until you are ready to be transferred to the ward.
After Surgery
Your nurse will check your blood pressure and pulse routinely. Your wound drain and wound will be checked for any bleeding and the urine output from your nephrostomy tube and catheter will be monitored closely. You will have a drip in your arm to make sure you receive adequate fluids. This will be removed once you are drinking normally. You can usually drink after surgery and you may eat once you are tolerating fluids.
Our aim is to keep you as comfortable as possible, it is important that the nurse know when the pain or discomfort starts so this can be treated and relieved as quickly and easily as possible. At all times, your nurse is there to help you, please ring your bell if you need assistance and a nurse is not nearby.
Day one after your operation
The morning after surgery the nurse will help you get up into a chair for a wash by the bedside or if you feel up to it you can go for a shower.
You will be given regular pain relievers, such as Panadol to help keep you comfortable.
You should do regular deep breathing and leg exercises after surgery until you are fully mobile. The physiotherapist may come and see you to give further instructions.
You will be up for a shower and about as able. Routinely, this is a very well tolerated procedure with minimal pain experienced. Our aim is to keep you comfortable, so please tell your nurse if you have any pain or discomfort so you can be given the appropriate care. At all times, your nurse is there to help you, please ring your bell if you need assistance and your nurse is not nearby.
Because recovery is quick, drains can be removed when drainage eases, often the next day or on day 2 when you will be able to go home. Even though the incisions are small and muscle damage is less, you are advised not to do any heavy lifting or strenuous activity for 2 – 3 weeks.
Day two or three after your operation
On the second or third day if the drainage from your wound drain is minimal it will be removed. Your catheter will also be removed if you are up and about and your urine output is sufficient. If you had a nephrostomy tube this would be clamped so that the urine can drain as it normally would from the kidneys down the ureter to the bladder. If you have no pain or wound leakage after clamping the nephrostomy it can be removed.
If you are comfortable on regular oral pain relievers, you will have your P.C.A. or epidural removed. The drip is not completely removed until the course of post-operative antibiotic treatment is complete.
Usually by the second or third day after surgery, all the drains and tubes have been removed. All the sutures used are dissolving so they do not need to be removed, however if wound staples are used these usually stay in for 7 to 10 days and are taken out by your own doctor or by the district nurse.
Going Home
Once your catheter, nephrostomy and wound drain have been removed and you are eating, drinking, and passing urine normally you will be able to go home. Before leaving the ward you will be given a discharge information letter which contains helpful information for when you get home.
You will be sent an outpatient appointment for 4 – 6 weeks after your operation. The stent that you had placed during your operation would usually be removed then, often after an x-ray dye study has shown that there are no urine leaks out of the new join in the ureter. Under local anaesthetic, a flexible telescope is passed up the urethra to the bladder so the end of the stent can be grasped and it can be removed.
We will send a letter to your own doctor about your operation and the details of your treatment while you were in hospital.
Once Home
Before discharge your nurse will inform you about taking mild pain relievers, should you have any pain or discomfort after you return home.
The internal healing after open surgery takes 3 – 4 weeks. During this time you should avoid any heavy lifting, straining or strenuous activity. Apart from strenuous activities you will be able to continue with your normal daily routines, as you feel able.
You should wash your wound with water only. No soap or powder is to be used directly on your wound until it is healed completely. Your wound would usually be dry within 48 hours of surgery; prior to this you will need to place a dry dressing over it daily after showering.
Contact your own doctor if:
- Your wound(s) become red, hot, swollen, painful or continues to discharge
- Your urine becomes cloudy, offensive smelling or you have any other signs of a urine infection
- You have any concerns at all
While you are in hospital, we will do everything we can to make your stay as comfortable as possible. The nursing and medical staff are always available to help with whatever needs you have. If you are worried about anything before or after your surgery, or if you have any further questions or would like more information, please do not hesitate to ask your nurse who will be more than happy to help.