- Men
- Bilateral Scrotal Orchidectomy
- Bladder Neck Incision (B.N.I.) and Urethrotomy
- Brachytherapy
- Circumcision
- Cystoscopy
- Flexible Cystoscopy
- Hydrocelectomy Spermatocelectomy & Epididymal Cystectomy
- Inguinal Orchidectomy
- Kidney Cryotherapy
- Laparoscopic Nephrectomy
- Laproscopic Pyeloplasty
- Laser Prostatectomy
- Magnetic Resonance Imaging (MRI) Scan
- Nephrectomy
- Orchidopexy
- Other Services (Men & Women)
- Other Treatments (Men Only)
- Robotic Assisted Laparoscopic Prostatectomy
- Sexual Dysfunction
- Transperineal Ultrasound Guided Prostate Biopsy (TPPB)
- Transrectal Ultrasound & Biopsies of the Prostate
- Transurethral Resection of Bladder Tumour
- Ureteroscopy
- Vasectomy
- Women
- Children
- Clinical Trials
Treatment Process:
Pubovaginal Sling
This information is designed to help you, your family and friends prepare for your surgery. It will also help you plan how to take care of yourself in the weeks following discharge from hospital.
What is a Pubovaginal Sling for?
This is an operation for urinary stress incontinence (leakage of urine without control), which usually occurs with any type of abdominal straining such as during exercise, coughing or sneezing. Stress incontinence is usually due to a weakness of the pelvic floor muscles and ligaments that no longer support the bladder neck. This lack of support causes the bladder to descend downward in the pelvis allowing urine to leak out. It can also be caused due to weakness of the sphincter (valve mechanism) that controls urine flow. Some of the causes for the weakness to the pelvic floor muscles and sphincter can be childbirth, having a hysterectomy and also hormone changes resulting from menopause. Being overweight also puts extra strain on the sphincter and will worsen your symptoms.
From the urodynamic bladder studies you have completed to find the cause of your incontinence, the Urologist has been able to determine that a sling would be the best surgery for you.
Treatment
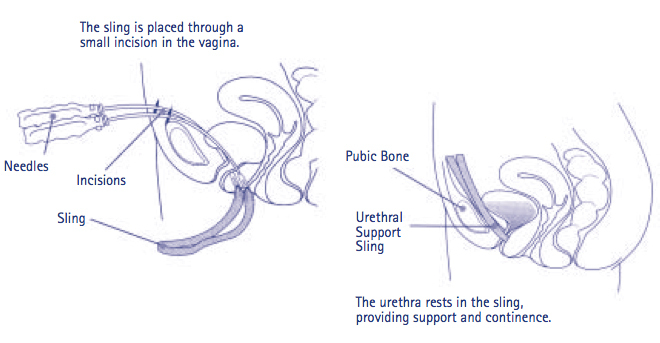
Two small incisions are made in the skin of the lower abdomen and one incision is made in the front wall of the vagina. A small channel is created on each side of the urethra and a special instrument is used to place the mesh sling under the urethra. The mesh will rest like a hammock under the urethra, supporting it during straining so there is no leakage of urine. The surgeon may then have a look into your bladder with a telescope to ensure the urethra is open and the bladder walls are intact. After this check, the mesh is trimmed to just below the skin surface and the wounds are closed.
A catheter may be left in place to drain the urine from your bladder into a collection bag. Gauze packing is sometimes used in the vagina to help minimise bleeding. The whole operation takes around 30 minutes to complete.
What can I expect after the operation?
After any operation there is always some swelling and discomfort but minimal following this technique due to the small size of the abdominal incisions.
If you have a catheter and / or vaginal packing, they are removed later in the day after theatre or the following morning. Once you have passed urine without difficulty you will be discharged home. You may find that emptying your bladder feels different and may be difficult. Normally, when you go to the toilet, you often push down or strain the abdominal muscles to empty the bladder. When doing this after surgery, the sling pulls against the urethra, which can close it off and stop the flow. Remember to take your time and just think about staying relaxed around your abdominal muscles. Leaning forward sometimes helps.
What are the risks involved with this operation?
Rarely, some women may not be able to empty their bladder satisfactorily or may be unable to void at all. In this case it is necessary to learn to pass a small catheter tube up into the bladder to empty it completely. This is called Intermittent Self-Catheterisation (ISC). This is done to reduce infection caused by urine not being flushed through regularly. The risk of having to do ISC following a sling is unlikely but needs to be considered.
Following this operation some women will experience an increase in frequency (the need to go to the toilet often) and urgency (the need to go to the toilet in a hurry). This is associated with irritability of the bladder following the operation. This will settle with time and perhaps the use of medication and bladder training (taught to you if required).
With all surgery there is a risk of infection and blood loss and there is always some bleeding involved with surgery. Antibiotics are often given during the operation to prevent infection and minimal bleeding is expected with this operation. You may have some light vaginal bleeding requiring a pad. Other bleeding such as bruising around the incision sites or haematoma (blood clot) under the surface of the skin are uncommon but will heal within 7-10 days.
Your Consent
We need your permission for the operation to go ahead. Before you sign the consent form it is important that you understand the risks and effects of the operation and anaesthetic. Your doctor and the nurse will discuss this with you. Should you have any questions, they would be happy to answer them.
It would be an extremely rare occurrence to require a blood transfusion with this surgery. However, in the unlikely event that you did need a blood transfusion and you want to refuse one, it is vital that you tell your surgeon and nurse prior to your surgery.
About Your Anaesthetic
You will NOT be allowed to eat or drink anything within 6 hours of your surgery. This includes chewing gum and sweets.
General anaesthetic: You will be asleep throughout and remember nothing about the operation.
Spinal anaesthetic: Is an option available under certain circumstances.
Your Operation
On admission, you will be told of your estimated operation time and will be fully prepared by your nurse. A shave of the operation sites is sometimes required, but this will be done in theatre while you are asleep.
You may be given some tablets to take before theatre. These are charted by the anaesthetist and may include tablets for tension, nausea and pain prevention. You will be escorted to the theatre where you will be transferred to the theatre table. Anaesthetic staff will then insert a drip in your hand or arm and will attach various monitoring devices. Once you have been given your anaesthetic and completely prepared, your surgery will begin. Operation time is around 30 minutes.
Once the operation is completed, you will go to the recovery room where you will be cared for until you are ready to be transferred to the ward. You may have a drip in your arm to make sure you get adequate fluids. This will be removed once you are tolerating fluids and you will be able to have something to eat.
Your urine may drain through your catheter from the bladder into a collecting bag.
If you had a spinal anaesthetic, you may have to lie flat for a while until it wears off. Otherwise you will be able to be up and about.
Our aim is to keep you as comfortable as possible, so please tell your nurse if you have any pain or discomfort so you can be given the appropriate care. At all times, if you need assistance and a nurse is not nearby, please ring your bell.
Going Home
You will be given a discharge information letter, which contains helpful information for when you go home and your nurse will inform you about taking mild pain relievers, should you have any discomfort when you go home.
You will be sent an outpatient appointment for follow-up, 4-6 weeks after your operation. We will also send a letter to your own doctor about your operation and the details of your treatment while you where in hospital.
Once Home
You should take regular mild pain relievers as instructed by the nurse prior to your discharge. This helps to keep you comfortable so you feel better.
Your abdominal wounds should heal in a few days. Normally the time off work would be 10-14 days at the most, depending on the type of work you do. During the time off work, you should avoid heavy lifting, preferably not more than 2-3 kg. Avoid becoming constipated by keeping up a good fluid intake and eating fruit and foods high in fibre. It is important not to strain the wall of the abdomen, because this may cause the leakage problem to return temporarily.
Avoid bathing and intercourse for 4 weeks so that the incision in the vagina has time to heal properly. The stitches may be visible from this wound but after some weeks, the stitches from the vagina can come out as small pieces as they dissolve. During this time you may get minor discharges from the vagina, which is completely normal.
Get in touch with your own doctor if:
- Your wound shows any signs of infection – becoming red, hot, swollen or excessively painful or has ongoing or mucky ooze.
- Your urine is offensive smelling, cloudy or you feel you may have a urine infection.
While you are in hospital, we will do everything we can to make your stay as comfortable as possible. The important thing is to remember that you are not alone. A positive attitude always aids in a speedy recovery and the nursing and medical staff are always available to help with any needs you may have. If you are worried about anything before or after surgery, if you have any further questions or would like more information, please do not hesitate to ask your nurse who will be more than happy to help you.